Hello and welcome to the Bangalore Spine Specialist Clinic blog! Today, we’re going to talk about a common spine condition that many people worry about: a bulging disc. You might have heard the term, or perhaps even experienced its symptoms. Our goal is to explain what a bulging disc is in simple, easy-to-understand language, and help you know when it’s time to see a specialist like Dr. Shashidhar B.K.
What Exactly is a Bulging Disc? Let’s Break It Down.
Imagine your spine – it’s not just one long bone. It’s made up of many individual bones called vertebrae, stacked on top of each other. Between each of these vertebrae, you have special cushions called intervertebral discs. Think of these discs like jelly donuts.
These discs have two main parts:
- A tough outer layer: This is like the dough of the donut, strong and fibrous.
- A soft, jelly-like center: This is the “jelly” inside, known as the nucleus pulposus.
The job of these discs is crucial! They act as shock absorbers for your spine, allowing it to move and flex, and protecting your vertebrae from grinding against each other.
Now, what happens with a “bulging disc”?
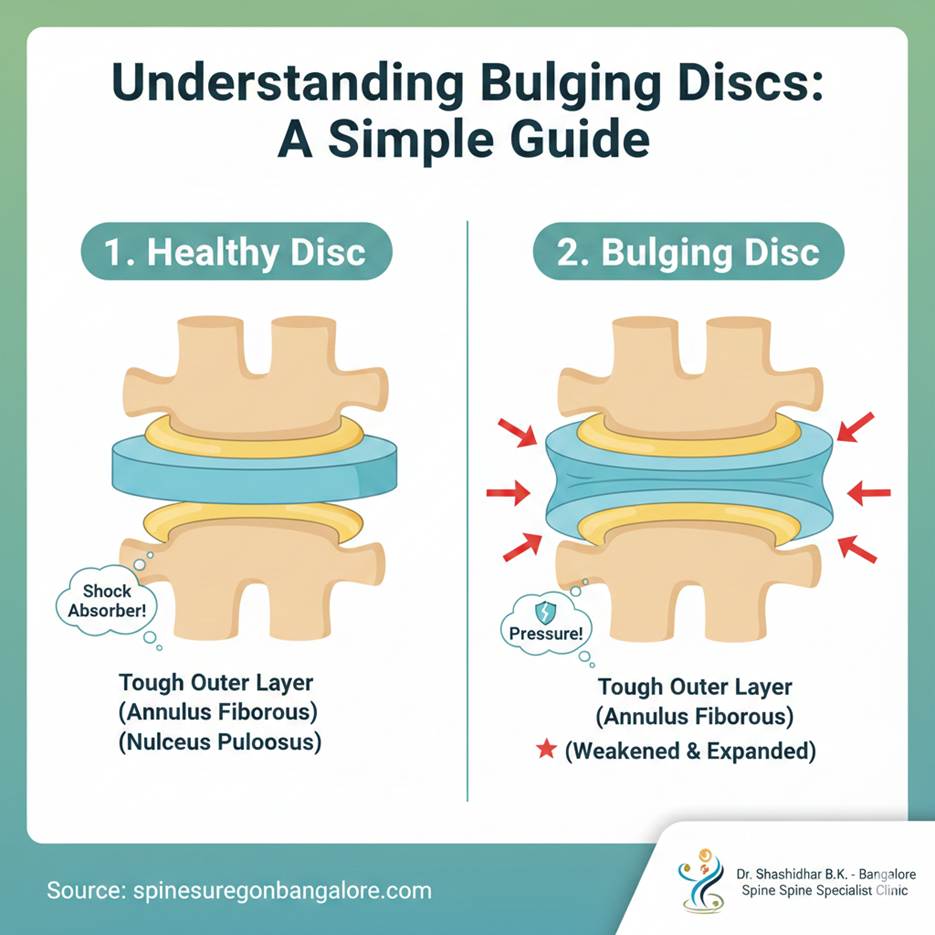
A bulging disc occurs when the tough outer layer of the disc starts to weaken and expand outwards, like a tire with a low pressure that bulges slightly at the sides. The soft, jelly-like center doesn’t necessarily push all the way through this outer layer, but the entire disc unit protrudes.
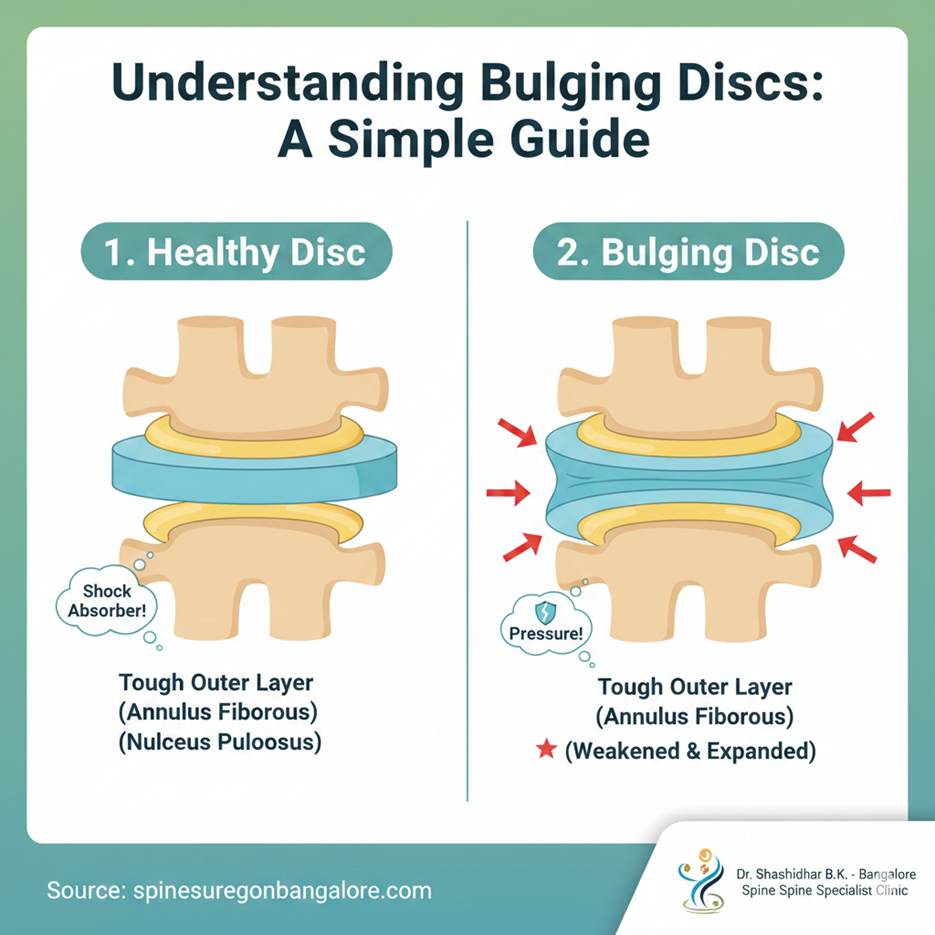
It’s important to understand that a bulging disc is often a natural part of aging and wear and tear on the spine. Think of it like wrinkles on your skin – they develop over time. Many people have bulging discs and don’t even know it because they experience no symptoms!
Bulging Disc vs. Herniated Disc: What’s the Difference?
You might also hear the term “herniated disc” or “slipped disc.” While similar, there’s a key difference:
- Bulging Disc: The entire disc wall weakens and bulges outward, but the jelly-like center remains contained within the outer layer.
- Herniated Disc: A crack or tear occurs in the tough outer layer, allowing some of the soft, jelly-like center to push out of the disc. This is more like the jelly actually squeezing out of a donut.
A herniated disc often causes more severe symptoms because the escaped “jelly” is more likely to directly press on nearby nerves.

What Causes a Disc to Bulge?
Several factors can contribute to a disc bulging over time:
- Aging: As we get older, our discs naturally lose some of their water content, becoming less flexible and more prone to bulging.
- Wear and Tear: Years of everyday activities, especially those involving heavy lifting, twisting, or repetitive movements, can put stress on the discs.
- Genetics: Some people are simply more predisposed to disc problems due to their genes.
- Injury: A sudden trauma, like a fall or car accident, can sometimes cause or worsen a disc bulge.
- Poor Posture: Slouching or maintaining incorrect posture for long periods can place uneven pressure on your spinal discs.
- Obesity: Excess body weight puts additional strain on the discs, particularly in the lower back.
Symptoms: When Does a Bulging Disc Become a Problem?
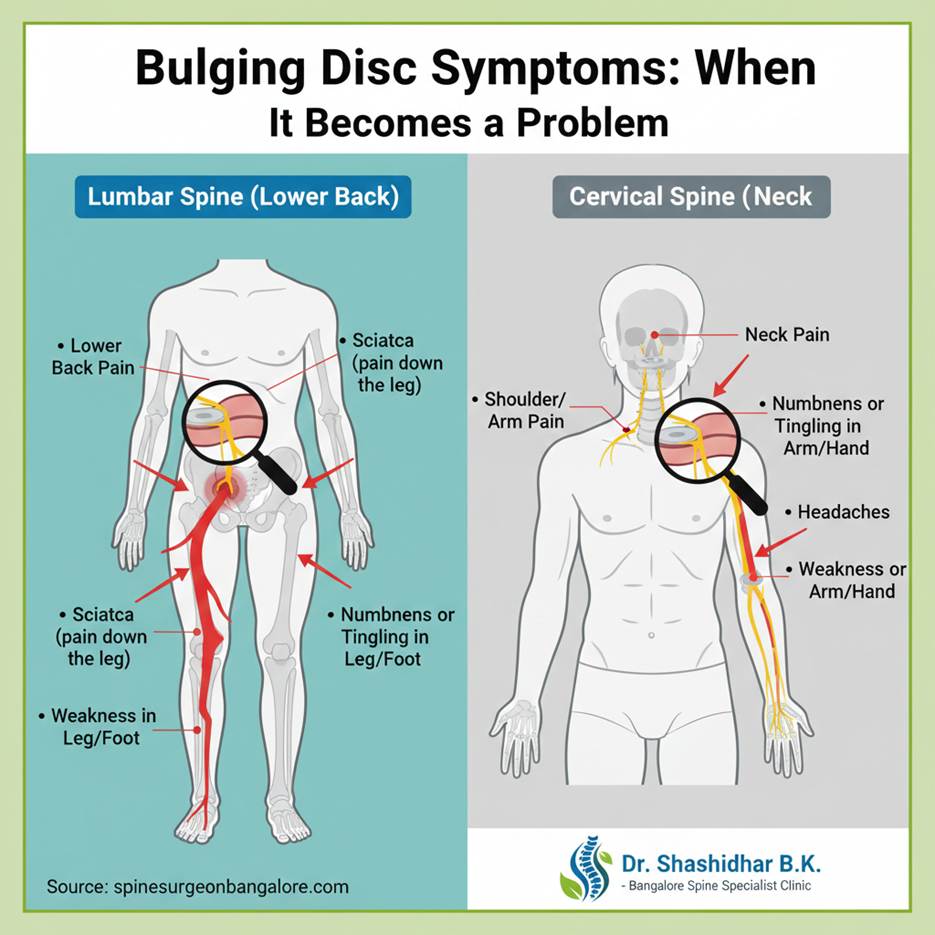
Remember, many bulging discs don’t cause any symptoms. Problems arise when the bulging disc presses on nearby nerves or the spinal cord. The symptoms depend on where the bulging disc is located in your spine:
- Lumbar Spine (Lower Back): This is the most common area.
- Pain: Often felt in the lower back, buttocks, thigh, and calf. This pain can range from a dull ache to a sharp, shooting sensation.
- Numbness or Tingling: A “pins and needles” sensation in the leg or foot.
- Weakness: Difficulty lifting your foot (foot drop) or weakness in certain leg muscles.
- Sciatica: This is a common term for pain that radiates along the path of the sciatic nerve, which runs from your lower back down each leg. It’s often caused by a bulging or herniated disc irritating this nerve.
- Cervical Spine (Neck):
- Neck Pain: Can be localized or radiate to the shoulder, arm, hand, or fingers.
- Numbness or Tingling: In the arm, hand, or fingers.
- Weakness: In the arm or hand.
- Headaches: Sometimes neck problems can lead to headaches.
When is Treatment Needed for a Bulging Disc?
Most bulging discs, even those causing mild to moderate pain, respond well to conservative (non-surgical) treatments. The key is to manage the pain, reduce inflammation, and improve your spinal health.
You generally need treatment if you are experiencing:
- Persistent Pain: If your pain doesn’t improve with rest, over-the-counter pain relievers, or activity modification after a few weeks.
- Radiating Pain, Numbness, or Tingling: Especially if these symptoms are traveling down your arm or leg (like sciatica). This indicates nerve irritation.
- Weakness: Any noticeable weakness in your arm, hand, leg, or foot. This is a more concerning symptom as it suggests significant nerve compression.
- Impact on Daily Life: If your symptoms are interfering with your ability to work, sleep, exercise, or perform everyday activities.
You need URGENT medical attention if you experience:
- Loss of Bowel or Bladder Control: This is a rare but serious symptom called Cauda Equina Syndrome and requires immediate medical intervention.
- Progressive Weakness or Numbness: If your symptoms are rapidly worsening or affecting both legs.
- Severe Pain: If the pain is excruciating and unrelieved by anything.
Treatment Options for Bulging Discs
When you visit a spine specialist like Dr. Shashidhar B.K., a thorough examination and possibly imaging tests (like an MRI) will be performed to accurately diagnose your condition. Based on the severity of your symptoms and the diagnosis, a personalized treatment plan will be created.
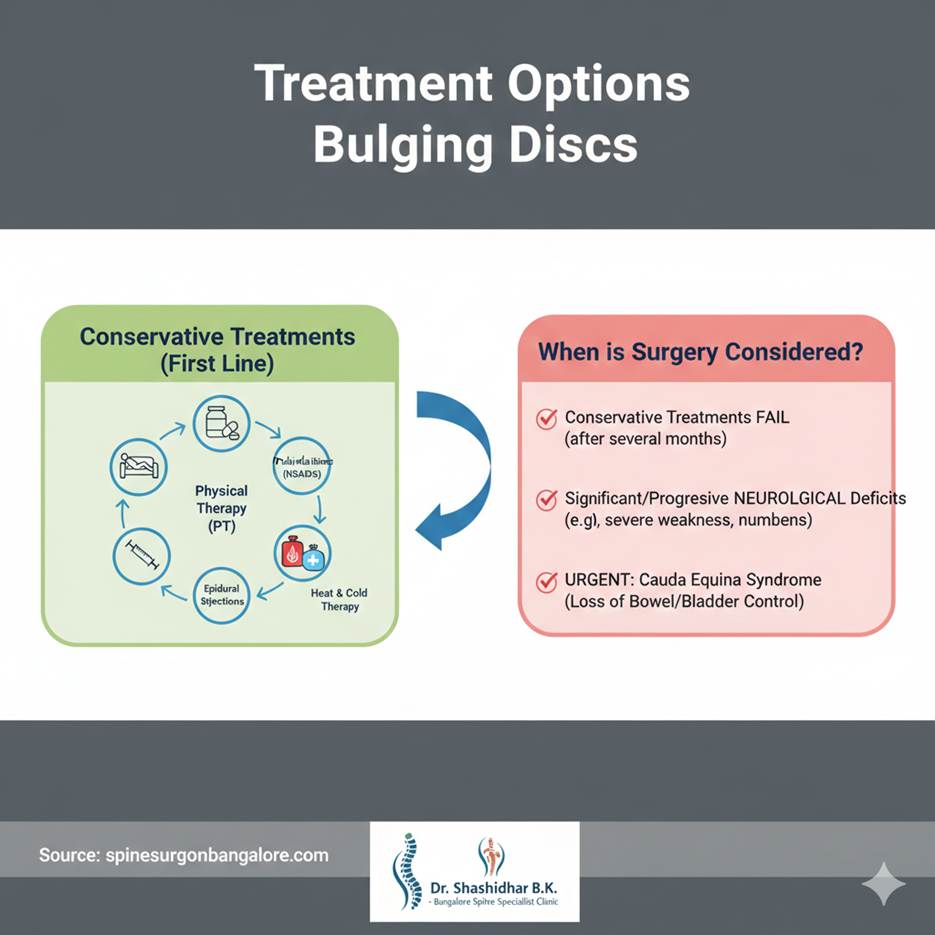
Most Common Treatments (Conservative):
- Rest and Activity Modification: Briefly reducing activities that worsen pain.
- Pain Medications: Over-the-counter pain relievers (like NSAIDs) or prescription medications for stronger pain and muscle spasms.
- Physical Therapy: A cornerstone of treatment! A physical therapist will teach you exercises to strengthen your core muscles, improve flexibility, and correct posture, which can significantly reduce pressure on your discs and nerves.
- Epidural Steroid Injections: In some cases, an injection of corticosteroids directly into the area around the affected nerve can reduce inflammation and provide significant pain relief.
- Heat and Cold Therapy: Applying heat or cold packs can help manage pain and muscle spasms.
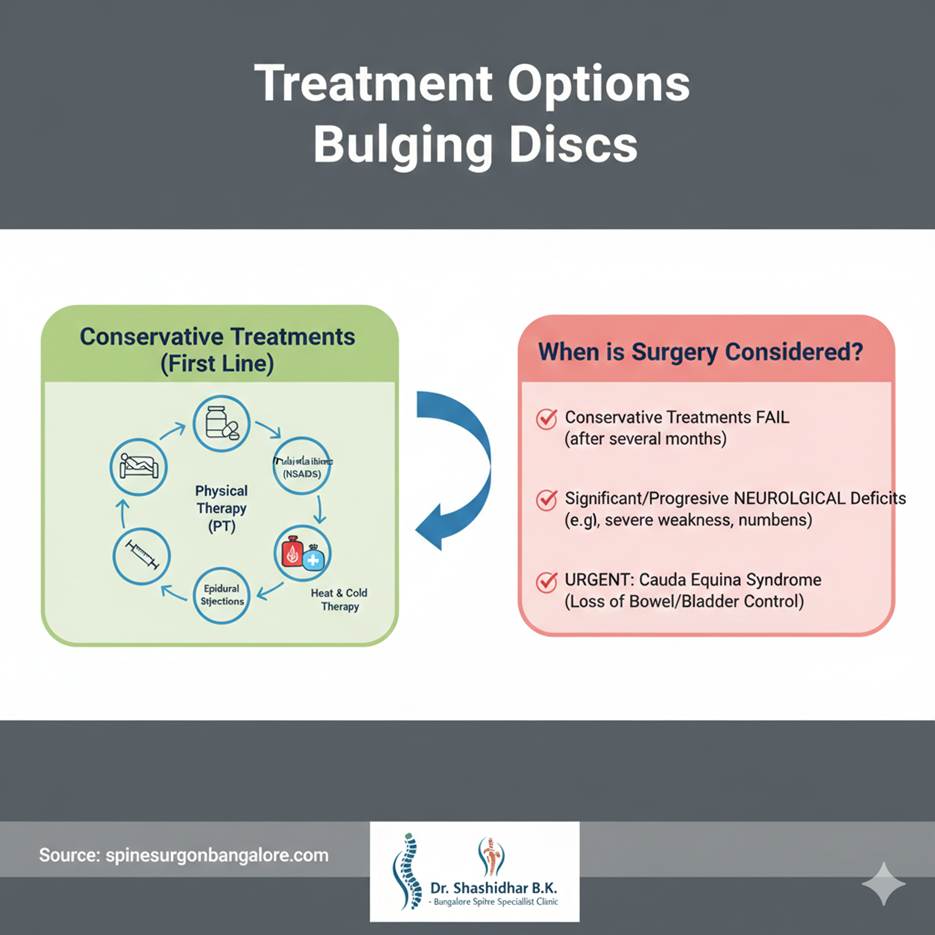
When is Surgery Considered?
Surgery is typically a last resort and is only considered if:
- Conservative treatments have failed to relieve symptoms after several months.
- You are experiencing significant or progressive neurological deficits (e.g., severe weakness, numbness, or loss of function).
- You have symptoms of Cauda Equina Syndrome (loss of bowel/bladder control).
The goal of surgery for a bulging disc (or more commonly, a herniated disc that is causing severe symptoms) is usually to remove the portion of the disc that is pressing on the nerve or spinal cord. Dr. Shashidhar B.K. specializes in advanced, minimally invasive spine surgery techniques that can offer effective relief with quicker recovery times when surgery is necessary.
Understanding Bulging Discs: A Simple Guide to When Treatment is Needed
Hello and welcome to the Bangalore Spine Specialist Clinic blog! Today, we’re going to talk about a common spine condition that many people worry about: a bulging disc. You might have heard the term, or perhaps even experienced its symptoms. Our goal is to explain what a bulging disc is in simple, easy-to-understand language, and help you know when it’s time to see a specialist like Dr. Shashidhar B.K.
What Exactly is a Bulging Disc? Let’s Break It Down.
Imagine your spine – it’s not just one long bone. It’s made up of many individual bones called vertebrae, stacked on top of each other. Between each of these vertebrae, you have special cushions called intervertebral discs. Think of these discs like jelly donuts.
These discs have two main parts:
- A tough outer layer: This is like the dough of the donut, strong and fibrous.
- A soft, jelly-like center: This is the “jelly” inside, known as the nucleus pulposus.
The job of these discs is crucial! They act as shock absorbers for your spine, allowing it to move and flex, and protecting your vertebrae from grinding against each other.
Now, what happens with a “bulging disc”?
A bulging disc occurs when the tough outer layer of the disc starts to weaken and expand outwards, like a tire with a low pressure that bulges slightly at the sides. The soft, jelly-like center doesn’t necessarily push all the way through this outer layer, but the entire disc unit protrudes.
It’s important to understand that a bulging disc is often a natural part of aging and wear and tear on the spine. Think of it like wrinkles on your skin – they develop over time. Many people have bulging discs and don’t even know it because they experience no symptoms!
Bulging Disc vs. Herniated Disc: What’s the Difference?
You might also hear the term “herniated disc” or “slipped disc.” While similar, there’s a key difference:
- Bulging Disc: The entire disc wall weakens and bulges outward, but the jelly-like center remains contained within the outer layer.
- Herniated Disc: A crack or tear occurs in the tough outer layer, allowing some of the soft, jelly-like center to push out of the disc. This is more like the jelly actually squeezing out of a donut.
A herniated disc often causes more severe symptoms because the escaped “jelly” is more likely to directly press on nearby nerves.

What Causes a Disc to Bulge?
Several factors can contribute to a disc bulging over time:
- Aging: As we get older, our discs naturally lose some of their water content, becoming less flexible and more prone to bulging.
- Wear and Tear: Years of everyday activities, especially those involving heavy lifting, twisting, or repetitive movements, can put stress on the discs.
- Genetics: Some people are simply more predisposed to disc problems due to their genes.
- Injury: A sudden trauma, like a fall or car accident, can sometimes cause or worsen a disc bulge.
- Poor Posture: Slouching or maintaining incorrect posture for long periods can place uneven pressure on your spinal discs.
- Obesity: Excess body weight puts additional strain on the discs, particularly in the lower back.
Symptoms: When Does a Bulging Disc Become a Problem?
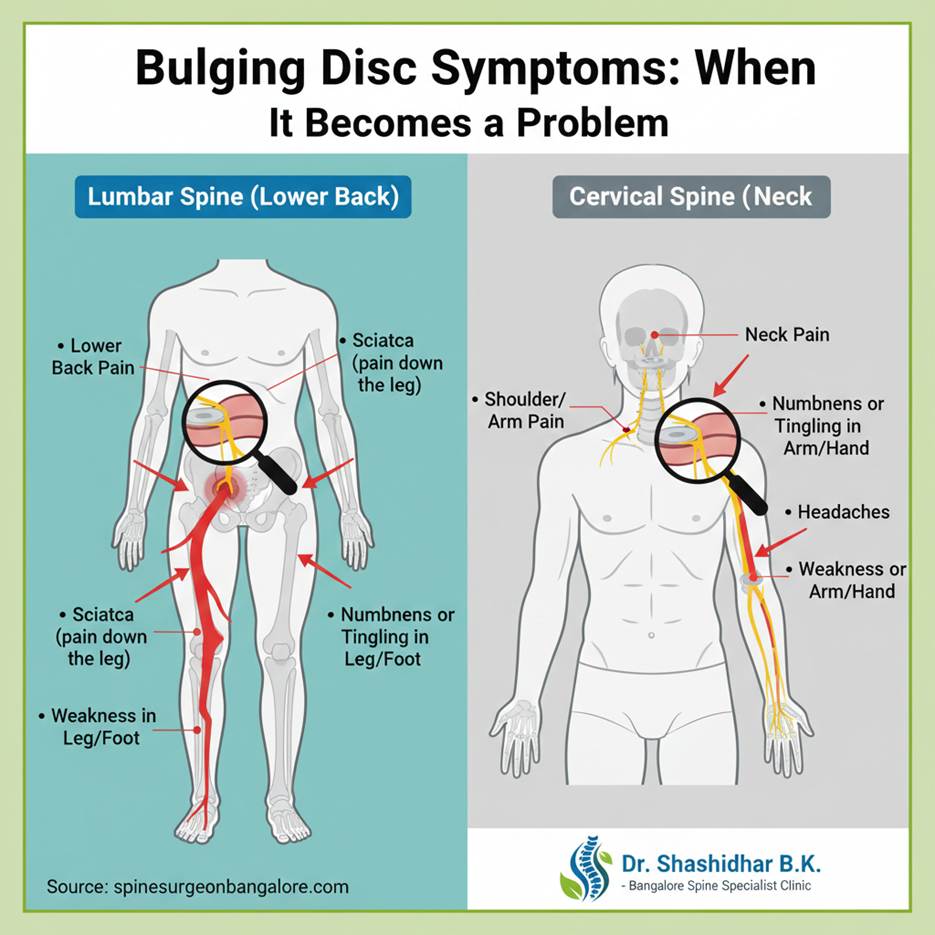
Remember, many bulging discs don’t cause any symptoms. Problems arise when the bulging disc presses on nearby nerves or the spinal cord. The symptoms depend on where the bulging disc is located in your spine:
- Lumbar Spine (Lower Back): This is the most common area.
- Pain: Often felt in the lower back, buttocks, thigh, and calf. This pain can range from a dull ache to a sharp, shooting sensation.
- Numbness or Tingling: A “pins and needles” sensation in the leg or foot.
- Weakness: Difficulty lifting your foot (foot drop) or weakness in certain leg muscles.
- Sciatica: This is a common term for pain that radiates along the path of the sciatic nerve, which runs from your lower back down each leg. It’s often caused by a bulging or herniated disc irritating this nerve.
- Cervical Spine (Neck):
- Neck Pain: Can be localized or radiate to the shoulder, arm, hand, or fingers.
- Numbness or Tingling: In the arm, hand, or fingers.
- Weakness: In the arm or hand.
- Headaches: Sometimes neck problems can lead to headaches.
When is Treatment Needed for a Bulging Disc?
Most bulging discs, even those causing mild to moderate pain, respond well to conservative (non-surgical) treatments. The key is to manage the pain, reduce inflammation, and improve your spinal health.
You generally need treatment if you are experiencing:
- Persistent Pain: If your pain doesn’t improve with rest, over-the-counter pain relievers, or activity modification after a few weeks.
- Radiating Pain, Numbness, or Tingling: Especially if these symptoms are traveling down your arm or leg (like sciatica). This indicates nerve irritation.
- Weakness: Any noticeable weakness in your arm, hand, leg, or foot. This is a more concerning symptom as it suggests significant nerve compression.
- Impact on Daily Life: If your symptoms are interfering with your ability to work, sleep, exercise, or perform everyday activities.
You need URGENT medical attention if you experience:
- Loss of Bowel or Bladder Control: This is a rare but serious symptom called Cauda Equina Syndrome and requires immediate medical intervention.
- Progressive Weakness or Numbness: If your symptoms are rapidly worsening or affecting both legs.
- Severe Pain: If the pain is excruciating and unrelieved by anything.
Treatment Options for Bulging Discs
When you visit a spine specialist like Dr. Shashidhar B.K., a thorough examination and possibly imaging tests (like an MRI) will be performed to accurately diagnose your condition. Based on the severity of your symptoms and the diagnosis, a personalized treatment plan will be created.
Most Common Treatments (Conservative):
- Rest and Activity Modification: Briefly reducing activities that worsen pain.
- Pain Medications: Over-the-counter pain relievers (like NSAIDs) or prescription medications for stronger pain and muscle spasms.
- Physical Therapy: A cornerstone of treatment! A physical therapist will teach you exercises to strengthen your core muscles, improve flexibility, and correct posture, which can significantly reduce pressure on your discs and nerves.
- Epidural Steroid Injections: In some cases, an injection of corticosteroids directly into the area around the affected nerve can reduce inflammation and provide significant pain relief.
- Heat and Cold Therapy: Applying heat or cold packs can help manage pain and muscle spasms.
When is Surgery Considered?
Surgery is typically a last resort and is only considered if:
- Conservative treatments have failed to relieve symptoms after several months.
- You are experiencing significant or progressive neurological deficits (e.g., severe weakness, numbness, or loss of function).
- You have symptoms of Cauda Equina Syndrome (loss of bowel/bladder control).
The goal of surgery for a bulging disc (or more commonly, a herniated disc that is causing severe symptoms) is usually to remove the portion of the disc that is pressing on the nerve or spinal cord. Dr. Shashidhar B.K. specializes in advanced, minimally invasive spine surgery techniques that can offer effective relief with quicker recovery times when surgery is necessary.