By Dr. Shashidhar. B.K, Consultant Spine Surgeon, Bangalore Spine Specialist Clinic, Bangalore
The human spine, a marvel of engineering, is the central pillar of our body, providing support, flexibility, and protection for the delicate spinal cord. It allows us to stand upright, twist, bend, and move with remarkable grace. Yet, this intricate structure is also susceptible to a wide array of ailments, from common wear-and-tear to more complex conditions, all of which often share a debilitating common denominator: pain.
For millions worldwide, spinal pain isn’t just a fleeting discomfort; it’s a persistent, often agonizing companion that disrupts daily life, steals sleep, and erodes quality of life. At Bangalore Spine Specialist Clinic, we understand the profound impact spinal pain can have. My team and I are dedicated to not just treating the underlying spinal condition, but fundamentally transforming the patient’s experience through comprehensive and personalized pain management strategies. This article aims to demystify the role of pain management in spinal ailments, empowering you, the layman, with knowledge about how modern approaches can lead to a life less burdened by pain.
Understanding Spinal Pain: More Than Just a Sensation
Before delving into management, it’s crucial to grasp what spinal pain truly is. It’s not merely a physical sensation; it’s a complex interplay of biological, psychological, and social factors.
- Acute Pain: This is the body’s alarm system, signaling immediate tissue damage or injury. A sudden sharp pain from lifting something heavy incorrectly, for instance, is acute. It typically resolves as the injury heals.
- Chronic Pain: When pain persists for more than three to six months, even after the initial injury has healed, it becomes chronic. This type of pain often develops a life of its own, impacting nerve pathways and even brain function. Chronic spinal pain can arise from conditions like degenerative disc disease, arthritis, spinal stenosis, or nerve compression.
- Neuropathic Pain: This results from damage or dysfunction of the nervous system itself. It’s often described as burning, tingling, shooting, or electric shock-like pain. Sciatica, caused by compression of the sciatic nerve, is a classic example of neuropathic pain originating from the spine.
- Nociceptive Pain: This is the more common type, stemming from actual or threatened damage to non-nervous tissue, such as muscles, ligaments, bones, or joints. It’s typically a dull ache, throbbing, or sharp pain.
Understanding these distinctions helps tailor the most effective pain management approach.
Why Traditional Approaches Often Fall Short
For many years, the primary approach to spinal pain was often simplistic: rest, medication (often strong painkillers), and sometimes, surgery as a last resort. While these elements have their place, they frequently fail to address the multi-faceted nature of chronic spinal pain.
- Over-reliance on medication: While crucial in acute phases, long-term dependence on pain medication can lead to side effects, tolerance, and addiction, without truly resolving the underlying issue.
- Lack of holistic perspective: Focusing solely on the physical symptom often ignores the psychological distress, fear, and functional limitations that accompany chronic pain.
- Delayed intervention: Waiting until pain becomes unbearable before seeking specialized care can make it harder to manage effectively.
This is where modern pain management steps in, offering a far more sophisticated and patient-centric approach.
The Pillars of Modern Pain Management for Spinal Ailments
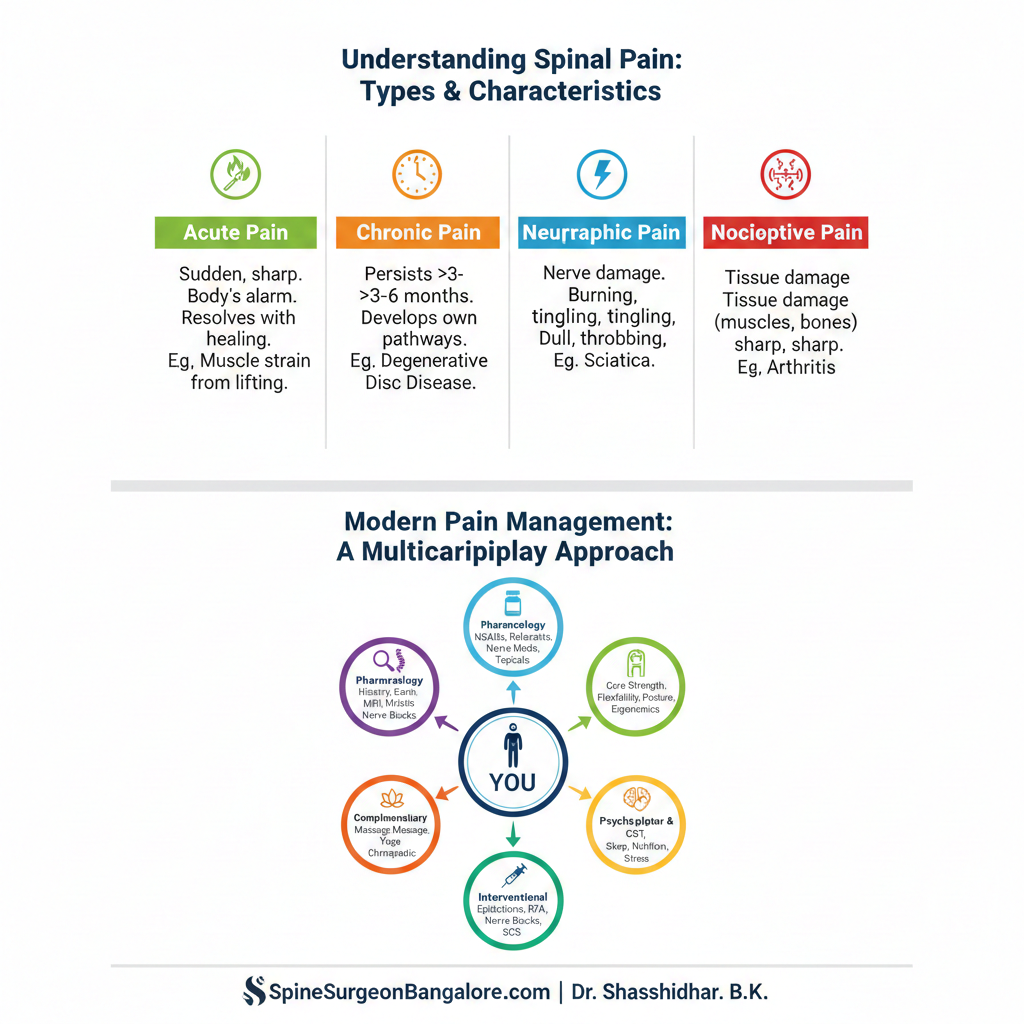
Modern pain management for spinal ailments is rarely a single treatment; it’s a carefully orchestrated symphony of therapies designed to reduce pain, improve function, and enhance quality of life. It’s about empowering the patient to take an active role in their recovery.
1. Accurate Diagnosis: The Foundation of Effective Treatment
Before any treatment begins, a precise diagnosis is paramount. This involves:
- Detailed Medical History: A thorough discussion about your pain, its onset, character, duration, aggravating and relieving factors, and impact on daily life.
- Physical Examination: Assessing posture, range of motion, muscle strength, reflexes, and sensory perception.
- Diagnostic Imaging: X-rays, MRI (Magnetic Resonance Imaging), and CT (Computed Tomography) scans provide detailed images of the spinal structures, helping to identify disc herniations, spinal stenosis, fractures, tumors, or degenerative changes.
- Electrodiagnostic Studies (EMG/NCS): These tests evaluate nerve function and can help pinpoint nerve compression or damage.
- Diagnostic Injections: In some cases, injecting a local anesthetic into a suspected pain source (e.g., a facet joint or nerve root) can confirm its role in generating pain.
2. Pharmacological Interventions: Targeted Relief
Medications are an important component, but they are used judiciously and strategically.
- NSAIDs (Non-Steroidal Anti-Inflammatory Drugs): Over-the-counter or prescription NSAIDs like ibuprofen or naproxen can reduce inflammation and mild to moderate pain.
- Muscle Relaxants: For muscle spasms often associated with spinal pain.
- Neuropathic Pain Medications: Drugs like gabapentin or pregabalin are specifically designed to calm overactive nerve signals in conditions like sciatica.
- Short-term Opioids: In severe acute pain or post-surgical situations, opioids may be used cautiously for a limited duration. Long-term opioid use is generally discouraged due to risks.
- Topical Agents: Creams, gels, or patches containing NSAIDs or local anesthetics can provide localized relief with fewer systemic side effects.
3. Physical Therapy and Rehabilitation: Restoring Function
Perhaps the most crucial non-surgical component of pain management, physical therapy focuses on restoring strength, flexibility, and proper movement patterns.
- Core Strengthening: A strong core (abdominal and back muscles) provides vital support to the spine, reducing strain.
- Stretching and Flexibility Exercises: Improve range of motion and reduce muscle stiffness.
- Posture Correction: Learning and maintaining correct posture can significantly reduce spinal stress.
- Ergonomics: Advice on how to perform daily activities (lifting, sitting, standing) in a spine-friendly manner.
- Modalities: Heat, cold, ultrasound, and TENS (Transcutaneous Electrical Nerve Stimulation) can provide symptomatic relief and facilitate exercise.
4. Interventional Pain Procedures: Precise Targeted Relief
When conservative measures aren’t enough, minimally invasive interventional procedures offer targeted relief by directly addressing the source of pain.
- Epidural Steroid Injections: Corticosteroids are injected into the epidural space (around the spinal cord and nerves) to reduce inflammation caused by disc herniation, stenosis, or nerve compression. This can provide significant, though often temporary, relief.
- Facet Joint Injections: The facet joints are small joints in the back of the spine that can become arthritic and painful. Injections of steroids and local anesthetic into these joints can diagnose and treat facet-mediated pain.
- Medial Branch Blocks: These are diagnostic injections used to determine if the facet joints are the source of pain. If successful, radiofrequency ablation may be considered.
- Radiofrequency Ablation (RFA): If medial branch blocks confirm facet joint pain, RFA uses heat generated by radio waves to “turn off” the nerves supplying the facet joints, providing longer-lasting pain relief (often 6-18 months).
- Nerve Blocks: Specific nerves causing pain (e.g., occipital nerves for headaches, sympathetic nerves for complex regional pain syndrome) can be blocked with local anesthetics.
- Sacroiliac (SI) Joint Injections: The SI joint connects the sacrum to the pelvis. If this joint is a pain generator, injections can provide relief.
- Spinal Cord Stimulators (SCS): For severe, persistent neuropathic pain (e.g., failed back surgery syndrome) that hasn’t responded to other treatments, SCS involves implanting a device that sends mild electrical pulses to the spinal cord, masking pain signals.
- Intrathecal Drug Delivery Systems (Pain Pumps): A small pump is surgically implanted to deliver pain medication directly into the spinal fluid, allowing for much lower doses and fewer side effects compared to oral medication.
5. Complementary and Alternative Therapies: Enhancing Well-being
Many patients find significant benefit from integrating complementary therapies into their pain management plan.
- Acupuncture: Involves inserting thin needles into specific points on the body to stimulate natural pain relief mechanisms.
- Massage Therapy: Can help relax tense muscles, improve blood flow, and reduce stress.
- Yoga and Tai Chi: Combine physical postures, breathing exercises, and meditation to improve flexibility, strength, balance, and mental well-being.
- Chiropractic Care/Osteopathy: Focus on spinal alignment and function. (Important to discuss with your spine surgeon to ensure suitability for your specific condition).
6. Psychological Support and Lifestyle Modifications: Addressing the Whole Person
Chronic pain often takes a toll on mental health, leading to anxiety, depression, and fear. Addressing these aspects is vital for comprehensive pain management.
- Cognitive Behavioral Therapy (CBT): Helps patients reframe negative thoughts about pain, develop coping strategies, and improve their ability to manage pain’s impact on their lives.
- Mindfulness and Meditation: Techniques to train attention and awareness, helping individuals observe pain without judgment and reduce its emotional impact.
- Stress Management: Chronic stress can exacerbate pain. Techniques like deep breathing, guided imagery, and progressive muscle relaxation can be beneficial.
- Sleep Hygiene: Poor sleep can worsen pain and fatigue. Addressing sleep issues is a critical part of recovery.
- Nutrition: A healthy, anti-inflammatory diet can support overall health and reduce inflammation.
- Smoking Cessation: Smoking significantly impairs spinal healing and increases the risk of disc degeneration.
When is Surgery Considered?
While pain management aims to prevent or delay surgery, it’s important to recognize that sometimes, surgical intervention is the most appropriate course of action. This is typically considered when:
- There is progressive neurological deficit (e.g., worsening weakness, numbness, or bowel/bladder dysfunction).
- Conservative pain management measures have failed to provide adequate relief for a significant period.
- There is clear structural instability or severe compression identified on imaging.
Even after surgery, pain management remains crucial. Post-operative pain protocols, physical therapy, and continued lifestyle modifications ensure optimal recovery and long-term success.
The Future of Pain Management: Precision and Personalization
The field of pain management is rapidly evolving, with a growing emphasis on precision medicine. Advances in genetic testing, artificial intelligence, and sophisticated imaging techniques are paving the way for even more personalized treatment plans. Regenerative medicine, including stem cell therapy and platelet-rich plasma (PRP) injections, also holds promise for certain spinal conditions, aiming to repair damaged tissues and reduce pain.
Takeaway Message for You, Our Patient
If you are suffering from spinal pain, please know that you do not have to endure it silently. The journey to relief begins with a comprehensive evaluation and an individualized pain management plan. At Bangalore Spine Specialist Clinic, my team and I are committed to working collaboratively with you, employing a multidisciplinary approach that considers all aspects of your pain and well-being. Our goal is not just to reduce your pain, but to help you reclaim your life, restore your function, and return to the activities you love.
Remember, effective pain management is a partnership. By actively participating in your treatment, adhering to recommendations, and communicating openly with your healthcare team, you empower yourself to achieve the best possible outcomes. Don’t let spinal pain dictate your life any longer. Seek expert care, and take the first step towards a pain-free, active future.
