A Guide for the Layperson
By Dr. Shashidhar B.K., Consultant Spine Surgeon, Bangalore Spine Specialist Clinic
The human spine is a marvel of engineering—a complex structure of bones, discs, muscles, and nerves that provides support, allows movement, and, most critically, protects the spinal cord. When this structure is compromised by severe deformity or disease, the consequences can be debilitating, affecting a person’s posture, mobility, and quality of life. In some of the most challenging cases, a highly specialized and technically demanding procedure known as Vertebral Column Resection (VCR) becomes the necessary path to correction and recovery.
If you or a loved one are facing a severe spinal condition, the term VCR might sound daunting. My goal in this article is to demystify this procedure, explaining in simple terms what it is, why it is performed, and what you can expect during the journey.
What is Vertebral Column Resection (VCR)?
Imagine the spine as a vertical stack of building blocks, the vertebrae. In a healthy spine, these blocks are perfectly aligned. However, due to severe conditions like congenital deformities, trauma, or certain types of tumors, one or more of these blocks might be severely misshapen or displaced, causing an extreme, rigid curvature.
Vertebral Column Resection, in essence, is the surgical procedure where a complete block of the spinal column, including the vertebral body, the posterior (back) elements, and the intervening discs, is carefully removed and then the gap is closed. This contrasts with other spinal procedures, which often involve removing only parts of the vertebra or fusing existing bones.
VCR is one of the most powerful and effective surgical techniques for correcting severe, rigid, and complex spinal deformities that cannot be corrected by less invasive methods.
The procedure is a last-resort option, reserved for spinal curves that are greater than $80^\circ$ and are too stiff (inflexible) to be corrected by simpler surgeries like an osteotomy.
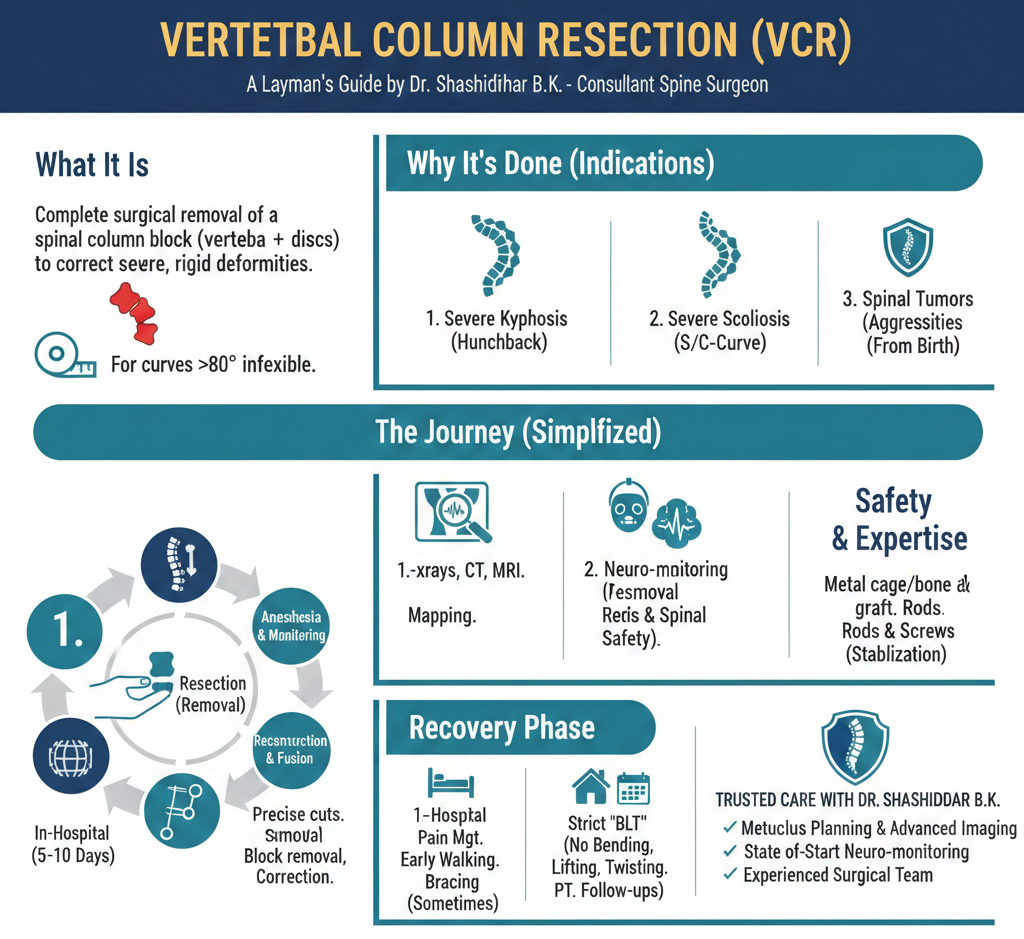
Why is VCR Performed? The Indications
VCR is not a procedure for common back pain or simple disc problems. It is reserved for specific, severe conditions where the deformity is causing significant problems, often threatening neurological function or vital organs.
1. Severe, Rigid Spinal Deformity (Kyphosis and Scoliosis)
The most common reason for VCR is the correction of extreme and rigid spinal curves, primarily:
- Severe Kyphosis (Hunchback): An excessive outward curvature of the spine, usually in the thoracic (mid-back) region. In severe cases, this can compress the chest cavity, affecting breathing, or cause persistent, debilitating pain.
- Severe Scoliosis (S- or C-shaped Curve): A sideways curvature of the spine. When the curve is very large, rigid, and causes the torso to collapse, VCR is used to straighten and rebalance the spine.
2. Spinal Tumors
VCR is sometimes performed to achieve a “clean margin” resection of aggressive tumors that are affecting the vertebral body and surrounding structures (e.g., chordoma or sarcoma). The goal is to remove the entire diseased section of the spine in one piece to reduce the chance of cancer recurrence.
3. Congenital Deformities
In children, VCR may be necessary to correct severe deformities present from birth, such as a hemivertebra (a condition where only half of a vertebral body forms).
The Surgical Journey: What Happens During a VCR?
VCR is one of the most complex procedures in spinal surgery, requiring a highly skilled team and meticulous planning.
1. Planning and Pre-operative Workup
Before the surgery, extensive imaging (X-rays, CT scans, and MRI) is performed. Dr. Shashidhar and the team will precisely map the curvature, identify the critical nerves, and determine the exact section of the spine that needs to be removed. Blood transfusions are often necessary, and the patient’s general health is thoroughly assessed.
2. Anesthesia and Monitoring
The patient is placed under general anesthesia. Throughout the procedure, a technique called Neurophysiological Monitoring is used. Small electrodes are placed on the patient’s limbs to continuously monitor the electrical signals traveling through the spinal cord. If the signals drop, the surgeon is immediately alerted, allowing for quick adjustments to prevent any nerve damage. This is a crucial safety measure.
3. The Resection (Removal)
The surgery is typically performed from the back (posterior approach), and sometimes also from the front (anterior approach), depending on the complexity.
- Exposing the Spine: The surgeon carefully exposes the vertebrae to be removed.
- Decompressing the Nerves: All nerves leading into and out of the area are meticulously identified and protected.
- The Cut: Using specialized surgical tools, the surgeon makes precise bone cuts above and below the diseased/deformed vertebra. The entire block is then gently and carefully removed. This is the moment of maximal correction.
4. Reconstruction and Fusion
A gap now exists where the removed vertebra used to be. The spine is now corrected and straightened. To maintain this correction and stabilize the spine, the gap is filled with a structural support, typically a metal cage (often titanium) or a bone graft.
- Instrumentation: Long, strong titanium rods and screws are placed on the vertebrae above and below the reconstruction site. These rods provide immediate, powerful internal fixation, holding the corrected spine rigid while the bone graft/cage integrates and heals (a process called fusion).
The overall goal is a stable, straight, and balanced spine.
The Recovery Phase: From Hospital to Home
Recovery from VCR is a significant commitment, but the potential for improved posture and reduced pain is a powerful motivator.
In the Hospital (5–10 Days)
- Initial Rest: The first few days are focused on pain management and careful monitoring of vital signs and neurological function.
- Mobilization: Physical therapists will begin early mobilization, often having the patient sit up and take a few steps with assistance within 3–5 days. This is essential for preventing complications and initiating the healing process.
- Bracing: In some cases, a custom-fitted brace may be recommended for several months to provide external support.
At Home (3–6 Months)
- Activity Restriction: The most important rule is to allow the fusion to heal. Patients must strictly avoid bending, lifting heavy objects, and twisting (the “BLT” restrictions) for the first few months.
- Physical Therapy: A structured physical therapy program will be necessary to rebuild core strength, improve flexibility, and restore mobility.
- Follow-up: Regular follow-up appointments with Dr. Shashidhar are essential to monitor the fusion process via X-rays and ensure a smooth recovery.
Safety and Expertise: Why Experience Matters
Vertebral Column Resection is a high-stakes procedure with potential risks, including infection, blood loss, or, most critically, neurological injury. This is why choosing a highly experienced and specialized spine surgeon is paramount.
As a dedicated Consultant Spine Surgeon at the Bangalore Spine Specialist Clinic, I prioritize:
- Meticulous Planning: Utilizing advanced imaging and surgical simulation to anticipate and mitigate risks.
- Advanced Neuromonitoring: Employing state-of-the-art technology and a specialized neuromonitoring team to safeguard the spinal cord throughout the surgery.
- Team Approach: Working with an experienced surgical and anesthesiology team trained to handle the specific demands of complex spinal procedures.
VCR offers a transformative opportunity for individuals suffering from severe spinal deformities. While the journey is challenging, the outcome—a straighter spine, improved balance, reduced pain, and a better quality of life—can be life-changing.
If you have been diagnosed with a severe spinal deformity and VCR has been suggested, I encourage you to seek a consultation to discuss your specific condition, the risks, and the highly personalized treatment plan we can offer. Your journey to a corrected and functional spine is within reach.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Please consult with a qualified spine specialist for diagnosis and treatment options.
